Top tips for Managers and Team Leaders
This set of tips for managers and team leaders are intended to help:
- build psychosocial resilience and wellbeing across teams
- manage team and individual stress and distress
- reduce risk of burn-out
- support those with additional mental health and wellbeing needs
1) Building psychosocial resilience and wellbeing

Stigma, perceived stigma and acknowledging emotional issues
- Managers, leaders and staff often worry that acknowledging emotions will hamper their promotion prospects
- Seeking help for problems (physical and mental) early on helps prevent them becoming serious and career impairing
- Sometimes of course, problems are serious. Whether they are physical or psychological, they can impact a person’s ability to do their job. This should not carry any stigma
- We want to build psychosocial resilience through seeking support early so that where possible we nip things in the bud. We should not be encouraging team members to be overly stoic with failing to seek help, and in turn, risking burn out
2) Leadership, team wellbeing, stress and distress
Command and Control
- A command-and-control style of leadership has its benefits at the right times and in the right circumstances. It may be appropriate in moments of crisis, for example
- A command-and-control model can give the impression of reliability ‘in the moment’
- However, if command-and-control approaches are applied to the management of psychological vulnerabilities in stressed-struggling staff it may impair problems being nipped in the bud, and someone’s wellbeing may well deteriorate
Principle and Values-based Leadership
As a leader you should:
- Help build a culture of wellbeing and psychosocial resilience within your team
- Demonstrate trustworthiness, transparency, and integrity. Specifically:
- strive to treat all members of the team fairly
- do not take on extra roles for the team in order to please your seniors when the team may not be able to safely carry them out
- communicate openly with your team about challenges which may affect their wellbeing and be responsive to concerns the team members might raise
- Manage and support staff with clarity of purpose, fairness and the aim of helping all to flourish in the workplace
- Be aware of the impact of you and your team members’ language, words, emotions and behaviours as the impacts are reciprocal and matter in teams
- Encourage the expression of positive emotions (e.g. gratitude, mutual support, determination, pride and optimism) even in difficult circumstances
- Acknowledge expected thoughts and feelings in a time like this (also known as validation). It helps people feel listened to. However, you need to also be aware of indicators of potentially more serious problems which need to be more fully assessed by you or another professional
- Help others to see that empathy and kindness in action can reduce tension and encourage cooperation in the team
- Make active efforts to overcome most people’s innate reluctance to speak about psychosocial wellbeing at work. Ensure you have the skills and confidence to have wellbeing focused conversations with your team
- Model calmness and compassion wherever you can, even in extreme situations
3) What else can I do to support the team as a leader?
Be a good role model
- Notice people’s strengths and speak about them
- Be honest, fair and transparent about the challenges and ambiguities staff are facing
- Buttress staff/teams for the challenges they face:
- Ensure safety and access to proper equipment
- Offer good supervision, regularly and when needed
- Make time for basic needs such as rest, food, and social connection
- Encourage ‘buddy-peer’ support within teams
- Allow time for questions from your colleagues
- Be aware of staff who are becoming vulnerable through work or home stress build ups. This means keeping up to date with key aspects of your team’s home lives
- Be aware of staff who are already vulnerable (eg., with pre-existing medical or mental disorders) and discuss with them what can be done to improve their situation
Decompression; post-event team reviews
- Decompression and structured (operational) post-event team reviews should be made routine. This is a good way to relieve the build-up of pressure during a shift through sharing and learning from each other
- These should follow the rules of no critiquing, and there should be no compulsion to speak but everyone should be given an opportunity to do so
- Ensure staff do not feel compelled to talk about experiences they do not feel ready to talk about
- The sharing has to be blame-free, reflective, kind and supportive. If you need to address poor performance, that should be done at another time
- Use what you say to open up sharing rather than shut it down. You will all learn more from each other this way
- This style cascades and helps foster compassion and positive attitudes to each other. It is sometimes called an operational team event review (debriefing is a term that can be misleading and result in unhelpful, overly psychologically focused approaches)
- Managers and team leaders should acknowledge their own limitations. They too may need to be looked after. Their wellbeing is a top priority; a stressed and burned-out leader will affect the wellbeing of all team members
Seek advice after stressful events from trusted peers, use buddy systems for team members and/or a mentor:
- Two minds can be better than one, especially when both people have walked in similar shoes
- Reflect carefully on what you say and what others say to you
Look out for signs of team stress. Early warning signs may include:
- Team members overworking and not attending to home or outside life
- Exhaustion
- Accidents
- Sick leave
- People becoming disengaged for example they may uncharacteristically fail to finish pieces of work
- Becoming irritable, arguing or increasing their use of unhealthy coping strategies such as cigarettes or alcohol
4) Supporting team members with additional mental health and wellbeing needs
Each service should have clearly defined pathways to access more specialised help and care.
- Information about these should be readily available.
- There should be anonymous ways of seeking help for those who are reluctant to initially engage
Here are three tools briefly summarised here to help you. These three tools could be embedded in your service-wide approach:
- The 5 Rs, a mnemonic to support relationships and psychosocial resilience
- The four principles of “PIES” for support after trauma
- Psychological First Aid (PFA) - simple ordinary steps for everyone
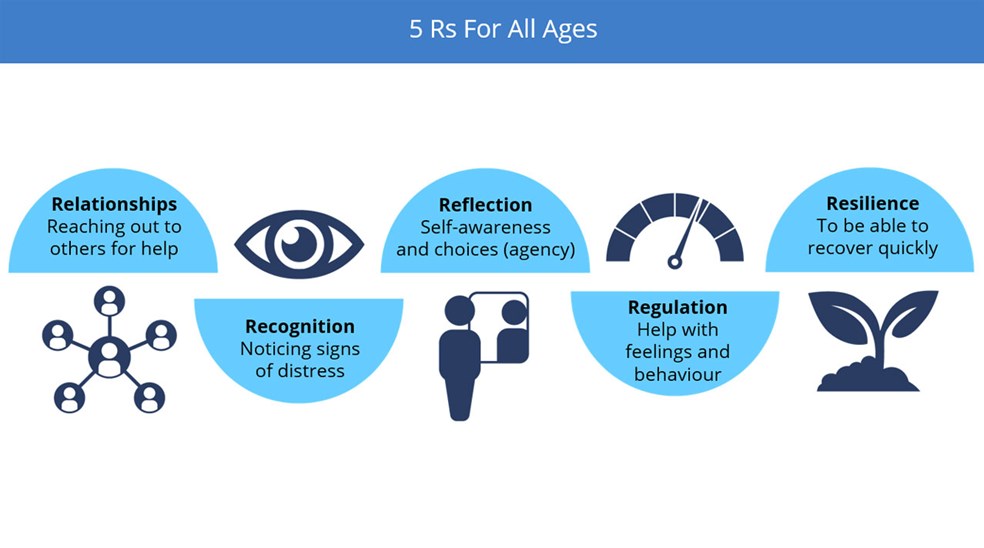
a) The Five Rs - a mnemonic to support relationships and psychosocial resilience
- This is a map, and mnemonic device, for the five key actions that will help your leadership and daily team working
- Remember to think about relationships, recognising distress, supporting reflection and self-awareness, supporting emotional regulation and building psychosocial resilience together
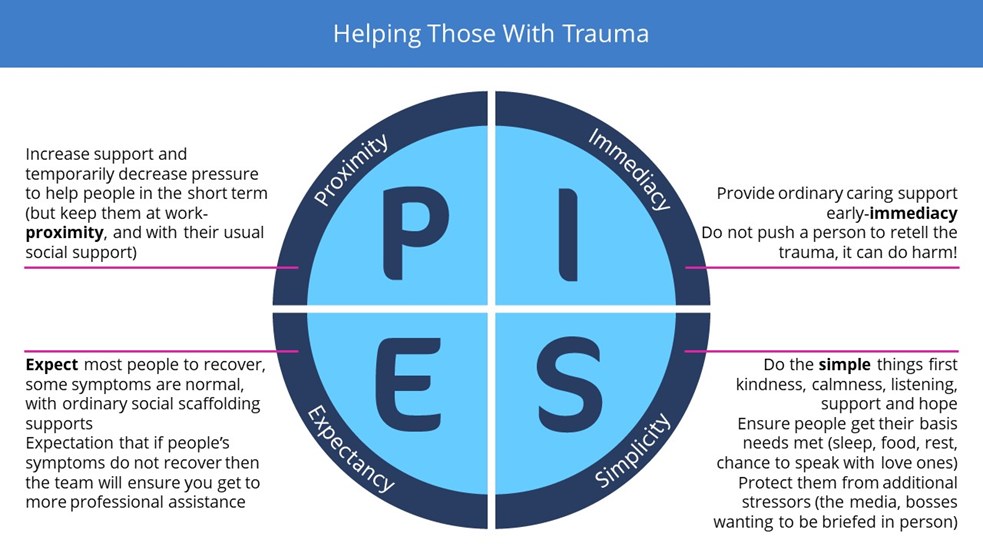
b) The four principles of “PIES” for support after trauma
-
- The four principles of PIES come from experience in the military. They can help you to provide quick support soon after a trauma
c) Psychological First Aid (PFA, World Health Organisation 2020)- simple ordinary steps for everyone
-
- Remember to look for signs of distress, listen and support, and consider further links and supports

-
- Use good listening skills

Each service should have clearly defined pathways to more specialised help and care
- Ensure access to occupational healthcare to enable staff in need to receive assessments of those needs
- Create service level agreements with agencies, that ensure ease of access for certain staff, to timely and reliable GP, and specialist mental healthcare
Resources and references
- Internally:
- Occupational Health
- External resources that may offer help:
- GP
- Improving Access to Psychological Therapies (IAPT)
- References:
- Jones, N, Fear N.T., Wessely, S., Thandi, G. and Greenberg, N. (2017) Forward psychiatry – early intervention for mental health problems among UK armed forces in Afghanistan European Psychiatry 39, 66-72
- Solomon Z, Mikulincer M. Trajectories of PTSD : A 20-year longitudinal study. American Journal of Psychiatry 2003 ; 1 63 : 659–666
- Stevenson D, Farmer P. Thriving at Work: The Stevenson/ Farmer Review of Mental Health and Employers. Department for Work and Pensions and Department of Health and Social Care; 2017
- Milligan-Saville JS, Tan L, Gayed A, Barnes C, Dobson M, Bryant RA, Christensen H, Mykletun A, Harvey SB. Workplace mental health training for managers and its effect on sick leave in employees: a cluster randomised control trial. Lancet Psychiatry 2017; 4: 850-85
- Other resources
- NHS Employers. NHS Staff Survey 2019. NHS Employers; 2020.
- Police Care UK. Policing: The job and the life survey Police Care UK; 2018
- Association of Chief Ambulance Officers. Supporting ambulance staff on mental health and wellbeing. Assocaition of Chief Ambulance Officers; 2019.
- College of Paramedics. Paramedic mental health and wellbeing: Your mental health. College of Paramedics; 2020.
- College of Paramedics. Guidance for managers on psychosocial support and mental wellbeing of ambulance personnel in a pandemic; 2020. Accessed 28 December 2020
- National Fire Chiefs Council. MIND Mental Health in the Emergency Services.
- Merseyside Fire and Rescue Authority. Critical Incident Stress Management; 2014
- Web resources:
- NHS People
- NHS Practitioner Health
- Psychological First Aid
- Mind: Blue Light Programme Research Summary 2016-18. London: Mind; 2018.
- March on Stress TRiM
- The Oscar Kilo Programme
- HeadFit - aimed at the military but trying to appeal to others too
- Critical incident stress management: Merseyside FRS
- MindEd Mindfulness e-learning session
- Other support groups and caring organisations you may find helpful include:
- The Samaritans – offers a 24- hour helpline for those in crisis. Tel: 116 123
- Cruse – Bereavement Care – Offers counselling, advice and support throughout the UK. Tel: 0808 808 1677
- Assist Trauma Care – Offers telephone counselling and support to individuals and families in the aftermath of trauma. Tel: 01788 551919.
- Drinkaware – offers facts, advice and support to manage drinking. Tel: 020 7766 9900
- Relate – offers relationship support for couples and families. Tel: 0300 0030396
- Stonewall – offers information, advice and support for gay, lesbian, bi, and trans communities. Tel: FREEPHONE 0800 0502020.
- Domestic Violence Intervention Project – offers advice and support to individuals and families who have experienced domestic violence as well as to individuals who want to change their behaviour. Tel: 020 7633 9181.
- The Ambulance Staff Charity (TASC)
- Our Frontline
- Just B
- Shout – Mental Health At Work
- College of Paramedics
- The Fire Fighters Charity - offers a range of mental and physical health support, as well as residential stays.
- Assist Trauma Care - provides information and help for people with PTSD and anyone supporting them
- PTSD999 - support and training for serving and retired emergency services personnel
Acknowledgements
The content for these tips draws upon four more detailed elearning sessions launched in 2021 for Blue Light Services Staff “Building Staff Psychosocial Resilience and Wellbeing”. We are grateful to the authoring teams for all their input and support, upon which these tips are built.
Previous Back to Blue Light Home
Disclaimer
This document provides general information and discussions about health and related subjects. The information and other content provided in this document, or in any linked materials, are not intended and should not be construed as medical advice, nor is the information a substitute for professional medical expertise or treatment.
If you or any other person has a medical concern, you should consult with your healthcare provider or seek other professional medical treatment. Never disregard professional medical advice or delay in seeking it because of something that you have read in this document or in any linked materials. If you think you may have an emergency, call an appropriate source of help and support such as your doctor or emergency services immediately.
MindEd is created by a group of organisations and is funded by NHS England, the Department of Health and Social Care and the Department for Education.
© 2023 NHS England, MindEd Programme



